
Fentanyl is a powerful synthetic opioid used in medicine for severe pain and, unfortunately, increasingly found in the illicit drug supply. 1 Knowing how long it stays in the body helps families, clinicians, and forensic teams interpret test results and manage safety.
This article outlines typical detection windows for different specimen types, summarizes fentanyl metabolism (including the norfentanyl metabolite), explains half-life and how it affects detectability, and reviews patient and drug factors that can slow clearance.
You’ll find practical, conservative ranges for urine, blood, saliva, hair, and nails, learn how test type and sensitivity change interpretation, and see when clinical evaluation is warranted.
What Is the Typical Fentanyl Detection Window in the Body?
Detection windows depend on the specimen tested and whether exposure was single or repeated. Fentanyl is quickly converted to norfentanyl and also distributes into tissues, so results vary: blood shows very recent use, saliva mirrors blood for recent exposure, urine detects metabolites for longer, and hair or nails reflect use over weeks to months.
If you’re worried about recent exposure or possible dependence, a healthcare professional can help assess symptoms and testing options. Below is a concise comparison of common specimens with conservative ranges for single-use and chronic use, while noting lab and individual variability.
| Specimen type | Typical Detection Window (single-use) | Typical Detection Window (chronic use) |
|---|---|---|
| Urine | 24–72 hours for (parent/metabolite) | Up to 7–10 or more days (metabolite accumulation) |
| Blood (plasma) | Up to 6–12 hours for (parent drug) | Up to 24–48 hours in some cases |
| Saliva (oral fluid) | 12–24 hours for (parent drug) | Up to several days, depending on use pattern |
| Hair (scalp) | Detects exposure after about 7–10 days; shows months of history | Can record chronic use for 90 days or longer |
| Nails | Weeks to months after exposure | Can reflect repeated exposure over months |
This table shows that urine and blood are best for detecting recent use, while hair and nails document longer-term exposure rather than exact timing. Test sensitivity, sample timing, and whether the lab looks for norfentanyl versus the parent drug can all shift these ranges.
Fentanyl Metabolism in the Body
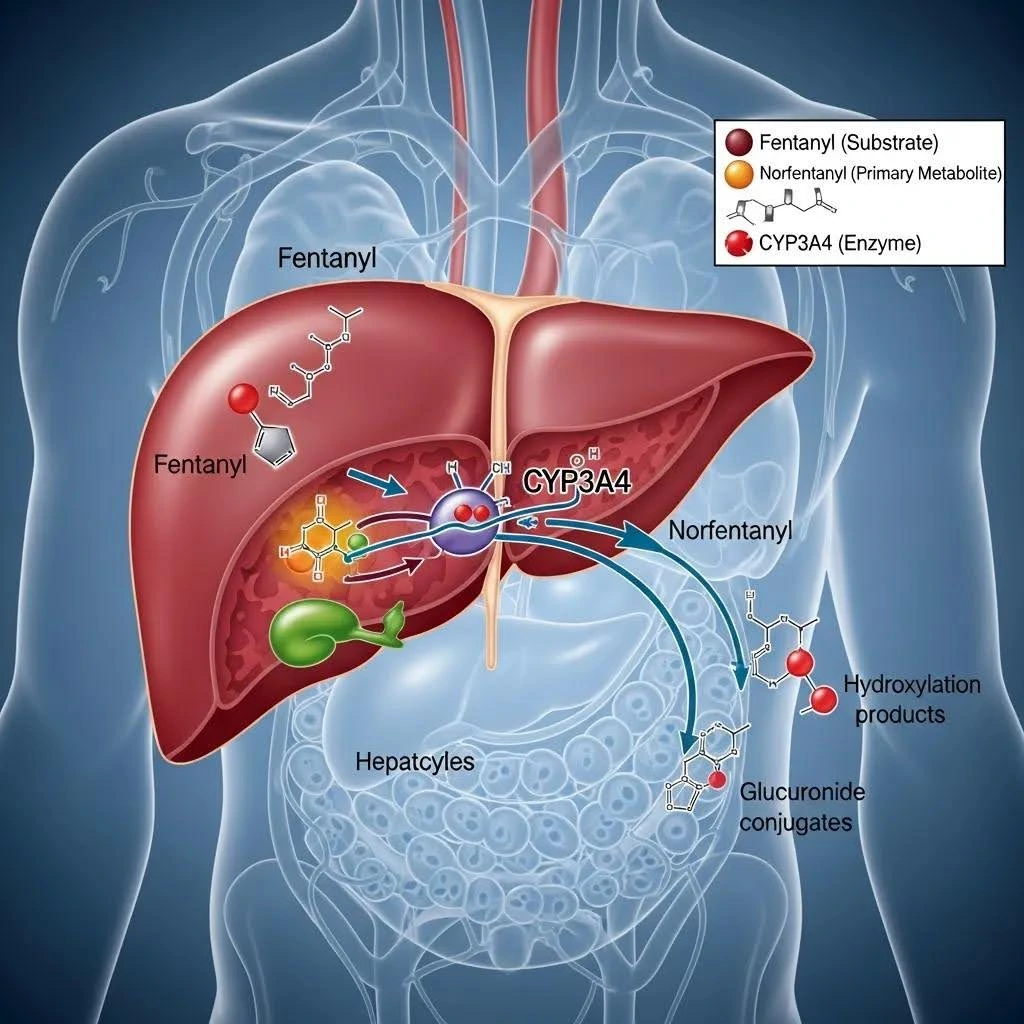
Fentanyl is metabolized in the liver primarily to norfentanyl, the metabolite that labs most often target to confirm exposure. The liver’s cytochrome P450 enzymes, especially CYP3A4, oxidize fentanyl to norfentanyl, which is then excreted mainly in urine. That pathway explains why drug interactions and liver disease can markedly slow clearance.
Some immunoassay screens detect parent fentanyl poorly and rely on confirmatory methods like GC-MS or LC-MS/MS that identify norfentanyl reliably. Because norfentanyl can persist after measurable parent drug levels drop, a urine sample may stay positive even when blood tests are already negative. 2
Factors Influencing Fentanyl’s Half-Life and Duration
Dose, route, frequency, and individual physiology all affect fentanyl’s effective half-life and how long it is detectable. 3 Larger or repeated doses increase tissue accumulation because fentanyl is lipophilic and stores in fat, creating a depot that prolongs elimination. 4
Transdermal patches produce longer apparent half-lives than a single IV dose due to continued absorption. Age, body composition, liver or kidney disease, and medications that inhibit or induce CYP3A4 will speed up or slow metabolism and change how long fentanyl and norfentanyl remain detectable.
What Is the Fentanyl Half-Life and How Does It Affect Detection?
Half-life is the time it takes for blood concentrations of a drug to fall by half and helps predict how long a drug will be detectable. Shorter half-lives usually mean faster clearance; longer or variable half-lives allow accumulation and longer detection windows with repeated dosing.
Reported fentanyl half-lives vary by route: IV bolus doses often show an effective half-life around 3–7 hours, while transdermal systems have a longer terminal phase because of ongoing absorption, sometimes extending to roughly 17 hours or more. 5
Because concentrations fall exponentially, it generally takes 4–5 half-lives before levels approach levels that are undetectable. Repeated use shortens the time to steady state and lengthens the time until levels fall below detection after stopping.
- Definition: Half-life reflects how quickly a drug is eliminated and helps predict how fast blood levels decline.
- Range: Fentanyl’s half-life typically spans several hours and is longer with transdermal delivery.
- Detection effect: Multiple doses cause accumulation, increasing how long the drug can be detected compared with a single dose.
That relationship is why chronic use can extend urine and hair detection windows beyond single-use estimates and why test timing is critical when interpreting results.
Fentanyl Urine Detection Time
Urine tests commonly detect norfentanyl and can stay positive longer than blood or saliva because metabolites are concentrated and eliminated in urine. Immunoassay screens vary in sensitivity; confirmatory GC-MS or LC-MS/MS testing identifies fentanyl and norfentanyl with higher specificity. 6
For a single exposure, a conservative urine detection window is about 24–72 hours; repeated or high-dose use can push that out to a week or more. Clinicians should interpret urine positives in light of timing, clinical signs, and the testing method, since assays that don’t target fentanyl metabolites can give misleading negatives.
Detection Windows in Blood, Hair, and Saliva
Blood testing is most useful for confirming very recent use and for forensic work in suspected overdose because fentanyl levels fall relatively quickly. Saliva (oral fluid) generally reflects blood for recent exposure and is easier to collect, but it’s less useful for long-term exposure.
Hair testing provides a retrospective record over months and can detect repeated use, but can’t precisely time individual doses. Each matrix has trade-offs: blood and saliva for recency, urine for metabolite-based detection, and hair or nails for long-term exposure profiling.
Which Factors Affect How Long Fentanyl Stays in the Body?
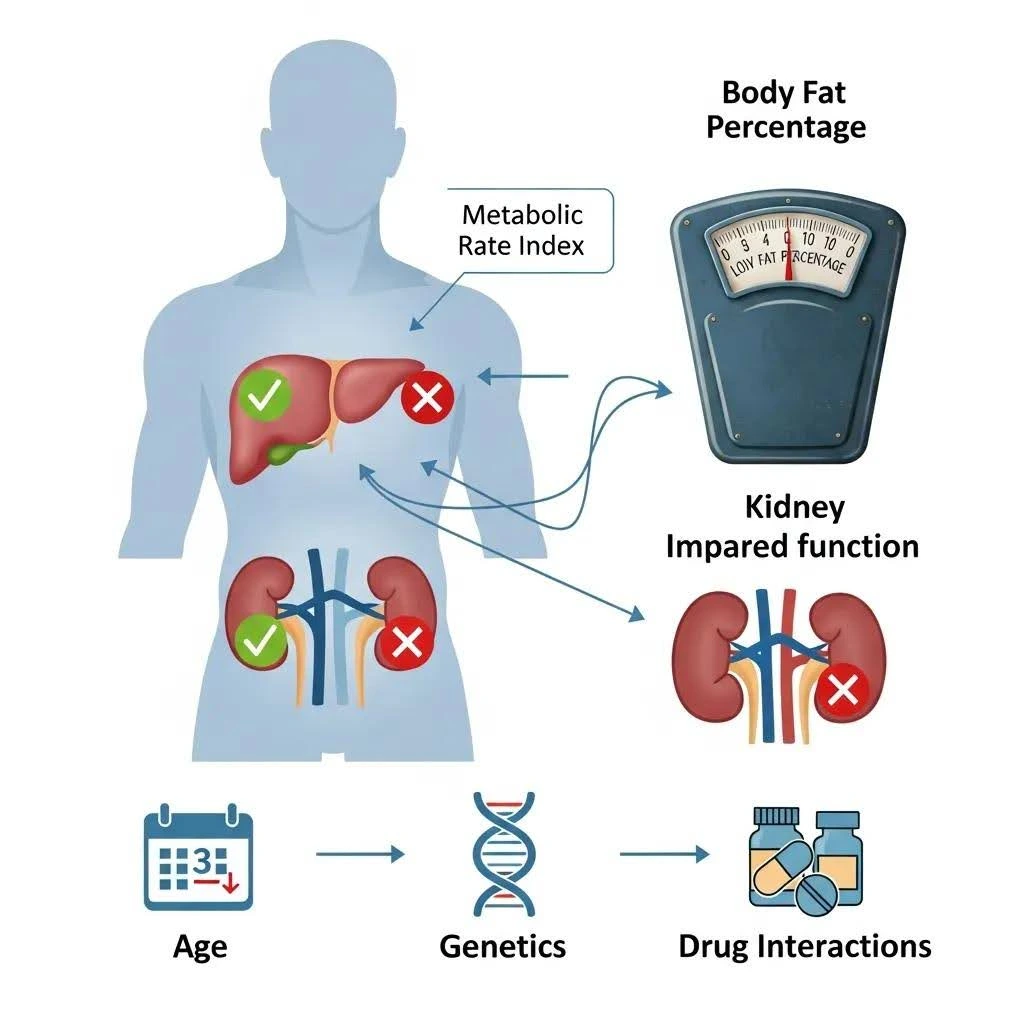
Biological and behavioral factors change fentanyl clearance and detection windows by altering distribution, metabolism, or excretion.
Major influences include dose and frequency, route of administration, body composition, liver and kidney function, age, and drug interactions that affect CYP3A4. These differences explain why two people with similar use may produce different test results and why clinical context is essential for interpretation.
Here’s how common factors modify detectability:
| Factor | Mechanism | Effect on Detection Time |
|---|---|---|
| Dose and frequency | Increased cumulative exposure and tissue loading | Lengthens detection window |
| Route of administration | Transdermal or repeated dosing extends the period of absorption | Extends apparent half-life |
| Body fat percentage | Lipophilic sequestration in adipose tissue | Slower release, prolonged detection |
| Liver function / CYP3A4 activity | Reduced metabolic conversion to norfentanyl | Slower clearance, longer detectability |
| Kidney function | Impaired excretion of metabolites | Prolonged urine detection |
This mapping makes clear that clinical variables either slow metabolism/excretion or increase storage in the body, both of which can extend how long tests stay positive and raise clinical risk.
If you or a family member is concerned about dependence, impaired metabolism, or repeated exposure, a professional assessment and timely treatment plan can make a difference. Providers can help arrange clinical evaluation, testing, and connection to appropriate care; contacting a local provider is a practical next step for anyone seeking support.
Norfentanyl Detection in Drug Testing
Norfentanyl is the main metabolite labs report to confirm fentanyl exposure, and it often extends the detection window beyond the parent drug. Because norfentanyl concentrates in urine, tests that include metabolite analysis are less likely to miss exposures than assays that only target fentanyl.
Laboratories typically report norfentanyl when using confirmatory GC‑MS or LC‑MS/MS, so clinicians should confirm whether metabolite testing is included when ordering tests. Recognizing the metabolite’s role helps avoid misinterpreting negative parent‑drug results.
Typical Detection Times for Norfentanyl
Estimated detection for norfentanyl generally matches or exceeds fentanyl’s urine window: single‑use detection often falls within 24–72 hours, while repeated or high‑dose exposure can extend detectability into multiple days. Hair and nail tests may also show norfentanyl as part of a longer exposure record.
Test sensitivity and when the sample is taken remain key caveats; a negative norfentanyl result doesn’t rule out very recent exposure if sampling missed the excretion peak.
How Long Does Fentanyl Remain Detectable in Different Drug Tests?
Different drug tests serve different clinical and forensic purposes. Choose the test based on whether the goal is to identify recent use, confirm exposure, or document long‑term patterns.
Urine immunoassays offer quick screening but vary in whether they detect fentanyl specifically or only broader opioid classes; GC‑MS and LC‑MS/MS confirmatory tests identify parent fentanyl and norfentanyl with high specificity. Below is a practical comparison of common test types and what labs typically detect.
| Test Type | What it Detects (parent vs metabolite) | Typical Sensitivity / Notes |
|---|---|---|
| Urine immunoassay | Often screens metabolites; some assays miss fentanyl unless fentanyl-specific | Rapid, variable sensitivity; positives generally need confirmation 7 |
| GC-MS / LC-MS/MS (urine or blood) | Detects parent fentanyl and norfentanyl | High specificity, used for confirmation |
| Blood (plasma) assays | Parent fentanyl primarily | Best for very recent use and overdose evaluation |
| Oral fluid (saliva) tests | Parent fentanyl is detectable shortly after use | Useful for near-term screening; less standardized across labs |
| Hair testing (GC-MS) | Parent and metabolite are incorporated into the shaft | Long-term exposure record; not precise for timing |
This comparison highlights that confirmatory mass‑spectrometry methods are the most reliable for distinguishing fentanyl from other opioids and for reporting metabolites that extend detectability.
Effects of Dosage and Frequency on Detection Times
Larger doses and repeated dosing lead to tissue accumulation and a longer terminal elimination phase, so detection windows lengthen with greater exposure.
Occasional single use may clear in days from blood and urine, while daily use can keep metabolites detectable for a week or more and leave a long-term signature in hair. Clinicians use reported dosing patterns to interpret positives, assess overdose risk, anticipate withdrawal, and plan treatment.
- Occasional use: Shorter detection, typically days in urine.
- Regular use: Accumulation leads to longer detectability and higher clinical risk.
- High-dose or transdermal: Extended absorption and release increase detection time.
This dose–response relationship shows why testing strategies and clinical responses must consider use patterns rather than relying on a single test result.
Impact of Body Composition and Organ Function on Fentanyl Clearance
Fentanyl’s lipophilicity means it partitions into fatty tissue, creating a depot that slowly releases the drug back into the bloodstream and delays complete elimination. Poor liver function reduces conversion to norfentanyl and slows clearance; reduced kidney function limits excretion of metabolites, prolonging urine detection.
These mechanisms mean older adults, people with hepatic or renal disease, and those taking interacting medications are more likely to show extended detectability and may need closer clinical monitoring.
If you or a family member needs help interpreting test results, arranging confirmatory testing, or discussing treatment options, a professional evaluation and testing‑guided plan can clarify next steps and support safety. Providers and information hubs can help with questions and admissions for those seeking personalized care.
Frequently Asked Questions
What Are the Signs of a Fentanyl Overdose?
Common signs of fentanyl overdose include extreme drowsiness or inability to wake, slowed or difficult breathing, and loss of consciousness. 8 You may also see pinpoint pupils, cold or clammy skin, and a weak pulse. If you suspect an overdose, call emergency services right away. Naloxone can reverse an opioid overdose if given promptly, having it on hand and knowing how to use it can save a life.
How Does Fentanyl Compare to Other Opioids in Terms of Potency?
Fentanyl is much more potent than many other opioids, including morphine and heroin, roughly 50 to 100 times stronger than morphine. That potency makes it effective for severe pain but also raises the risk of overdose, especially when it’s present in illicit drugs where dose and purity are unknown.
Can Fentanyl Be Detected in Standard Drug Tests?
Fentanyl can be detected, but test performance depends on the method. Many urine immunoassays will detect fentanyl-related compounds, though some screens only identify broader opioid classes. Confirmatory tests like GC‑MS or LC‑MS/MS are more reliable for identifying both fentanyl and norfentanyl. If you have a prescription for fentanyl, tell the testing facility to avoid misinterpretation.
What Should I Do if I Suspect Someone is Using Fentanyl?
Approach the situation with care. Encourage the person to seek professional help; fentanyl use can lead to dependence and overdose. Offer information about local treatment resources and support groups. If you think they are in immediate danger from an overdose, call emergency services at once. Early intervention and compassionate support are critical.
Disclaimer:
This article is for general information only and does not replace professional medical, legal, financial, or insurance advice. Policies, prices, and coverage vary. Always consult qualified professionals and your specific provider before making decisions.
Reference
- https://nida.nih.gov/research-topics/fentanyl
- https://www.bu.edu/aodhealth/2020/12/28/fentanyl-and-norfentanyl-detected-in-urine-for-7-or-more-days-after-regular-use/
- https://www.ncbi.nlm.nih.gov/books/NBK554498/
- https://pmc.ncbi.nlm.nih.gov/articles/PMC10593981/
- https://www.accessdata.fda.gov/drugsatfda_docs/label/2005/19813s039lbl.pdf
- https://www.mayoclinicproceedings.org/article/S0025-6196(16)30825-4/fulltext
- https://www.aafp.org/pubs/afp/issues/2019/0101/p33.html#article-comment-area
- https://www.aafp.org/pubs/afp/issues/2019/0101/p33.html#article-comment-area

