
Detoxing from alcohol means clearing alcohol from the body while stabilizing vital signs and managing withdrawal. 1 Faster stabilization is safest when guided by clinicians, not by trying to rush the process alone.
This page explains how a medically supervised alcohol detox shortens dangerous withdrawal periods, which symptoms need immediate care, and realistic timelines for quick but safe recovery.
You’ll find an evidence-informed 3–7 day core timeline, key red flags such as seizures and hallucinations, practical self-care steps that support stabilization, and how a licensed program coordinates care from intake through transition to ongoing treatment.
What Is the Typical Alcohol Detox Timeline for a Quick, Safe Recovery?
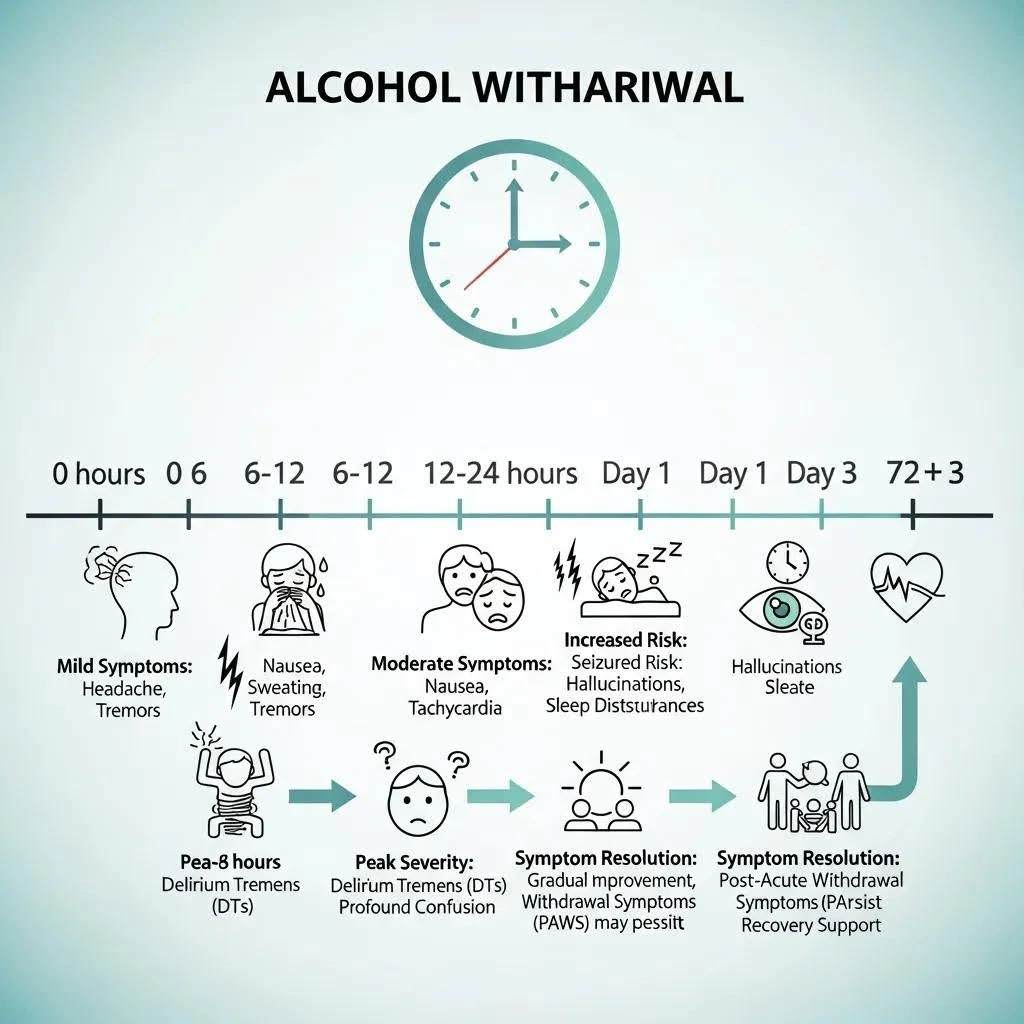
A typical alcohol detox follows early, peak, and resolution phases. With medical monitoring, clinicians can blunt dangerous peaks and speed safe stabilization. Early withdrawal often starts within 6–24 hours after the last drink. Symptoms commonly peak around 24–72 hours, and most major acute symptoms settle within 3–7 days, though some mild symptoms can linger. 2
Knowing these time points helps patients and families prepare and seek medical alcohol detox when withdrawal severity or co-occurring health issues increase risk. The timeline below summarizes common stages and symptoms so caregivers and clinicians can prioritize monitoring and medication when needed.
Withdrawal progresses in predictable stages with typical symptom clusters.
| Stage | When it Usually Occurs | Typical Symptoms & Severity |
|---|---|---|
| Early (mild) | 6–24 hours | Anxiety, hand tremors, headache, nausea |
| Peak (moderate–severe) | 24–72 hours | Elevated blood pressure, rapid heart rate, strong tremors, hallucinations, seizure risk |
| Acute resolution | 3–7 days | Symptoms ease; stabilization is achieved with medical support |
This table highlights when monitoring and intervention matter most and how medical detox can narrow the window of highest risk.
Physical and Psychological Symptoms That Indicate Medical Detox Is Needed
Certain physical and psychological signs mean someone should receive medically supervised detox rather than attempting it at home. Red flags include high fever, a very rapid heartbeat, repeated vomiting, severe disorientation, visual or tactile hallucinations, and any history of seizures, all of which suggest a high risk for severe alcohol withdrawal, including delirium tremens. 3
Mental health symptoms such as intense agitation, suicidal thoughts, or overwhelming anxiety also require urgent clinical evaluation because they can threaten safety and complicate medical care. 4
Spotting these warning signs early allows prompt transfer to a medical setting where regular vital-sign checks and medication strategies can reduce risk and support recovery.
How Long Do Alcohol Withdrawal Symptoms Usually Last?
Duration of alcohol withdrawal symptoms depends on drinking history, severity, and other health conditions, but there are common timing anchors to guide expectations.
Mild symptoms can begin within hours and may be managed with outpatient support for some people. The highest-risk window for seizures and delirium tremens is the first 24–72 hours, so people at higher risk usually need inpatient observation. 5
With appropriate medical care, most acute and dangerous symptoms resolve within 3–7 days; sleep problems, mood changes, or anxiety may continue for weeks or months. 6 Understanding these timeframes helps families plan for monitoring, care escalation, and the next steps in treatment after detox.
Why Is Medical Alcohol Detox Essential for a Quick, Safe Recovery?
Medical detox is essential because clinical monitoring and evidence-based interventions lower the chance of life-threatening complications while promoting faster physiologic stabilization. Supervised detox includes ongoing assessment, medication-assisted treatment when needed, and correction of dehydration or electrolyte problems.
Together, these interventions reduce dangerous spikes in withdrawal and create a safer, more predictable timeline for discharge or transfer. Trying to speed detox at home removes these safeguards and raises the risk of seizures, severe autonomic instability, and delayed emergency treatment.
Unsupervised detox can quickly become a medical emergency that requires hospital-level care.
- Seizures are most likely in the first 24–72 hours and can cause serious injury or death.
- Delirium tremens can produce high fever, severe confusion, hallucinations, and cardiovascular collapse.
- Severe dehydration and electrolyte imbalance can damage the heart and kidneys.
Because of these risks, clinicians recommend medical alcohol detox for people showing moderate to severe withdrawal symptoms and stress the importance of early evaluation.
Risks of Detoxing from Alcohol at Home
Detoxing at home removes continuous monitoring and rapid medical response, increasing the chance of severe outcomes. Without regular vital-sign checks and professional assessment, warning signs such as accelerated heart rate or worsening tremors can be missed until seizures or delirium tremens occur.
Attempting detox at home also limits access to controlled medication tapering, seizure prevention, and nutritional or hydration interventions that reduce complications. 7 Seek emergency care immediately for uncontrollable vomiting, loss of consciousness, seizures, or severe disorientation.
How Medical Detox Treats Withdrawal Symptoms
Medical detox combines ongoing monitoring, targeted medications, and supportive care to shorten dangerous windows and stabilize patients.
Clinicians perform frequent assessments, use proven medications when indicated to prevent seizures and severe autonomic reactions, and provide IV fluids or oral repletion to correct electrolytes.
Psychological support, sleep-promoting protocols, and gentle activity guidance reduce agitation and help restore normal sleep, all of which speed physical recovery. This integrated approach lowers complication rates and prepares patients for continued addiction treatment after detox.
How Charles River Recovery’s Medically Supervised Alcohol Detox Program Helps You Detox Quickly and Safely
At Charles River Recovery, our medically supervised alcohol detox in Massachusetts focuses on rapid stabilization without sacrificing safety or continuity of care. We combine licensed clinical monitoring, evidence-based medication strategies, nutritional and hydration support, and individualized discharge planning to shorten dangerous peaks and prepare patients for residential or outpatient treatment as needed.
Our team adjusts timelines based on medical assessment and screening for co-occurring disorders, so progress is both fast and safe. Program elements are designed to meet urgent medical needs and create a smooth path to ongoing care.
| Program Component | What It Does | Patient Benefit |
|---|---|---|
| Medical monitoring | Frequent vitals and clinical checks | Early detection and prevention of complications |
| Medication management | Evidence-based medications as needed | Lowers seizure and DT risk for quicker stabilization |
| Nutritional & hydration support | Restores electrolytes, fluids, and calories | Boosts physical resilience and speeds recovery |
This component-by-benefit view shows how coordinated services support a safer, more efficient detox and prepare patients for the next phase of treatment.
Stages of Alcohol Detox, From Intake to Transition
Detox generally moves through stages that we structure to accelerate stabilization while maintaining safety. Intake begins with a medical evaluation and baseline labs to identify risks and co-occurring conditions. During acute stabilization, we use monitoring and medications to control symptoms. 8
Once vitals and symptoms stabilize, staff implement tapering or symptom-targeted therapy, provide nutritional support, and address behavioral stabilization before planning discharge. Each stage has an expected timeframe but remains flexible to each patient’s needs, balancing speed with clinical judgment.
Personalized Detox Timelines at Charles River Recovery
Every timeline is individualized. Drinking history, age, medical issues, and other substance use change how quickly someone can detox safely. Our assessments determine whether a patient can move through detox quickly with close monitoring or needs longer inpatient stabilization before stepping down to residential or outpatient care.
Clear communication with families and a tailored transition plan reduces delays and helps patients make progress after detox. This personalized approach allows rapid stabilization without sacrificing clinical safeguards.
How to Manage Alcohol Withdrawal Symptoms Safely During a Quick Detox
Safe symptom management pairs prompt medical evaluation with practical self-care that supports the body and reduces discomfort. The top priority is a medical alcohol detox evaluation when symptoms are moderate or severe.
Clinical monitoring and medication-assisted treatment are the most effective ways to shorten dangerous peaks. Complementary self-care, adequate hydration, gentle nutrition, rest, and a calm environment help the body between clinical assessments. 9
- Seek medical evaluation promptly: A clinician will assess risk and determine the appropriate level of care.
- Drink fluids with electrolytes: Proper hydration reduces dizziness and corrects imbalances.
- Eat small, frequent protein-rich snacks: Stable blood sugar supports energy and recovery.
- Remain in a low-stimulation, supervised setting: Less agitation lowers seizure risk and helps sleep return.
Helpful Foods and Hydration Practices During Alcohol Detox
Simple nutrition and hydration can help reduce common complications, such as low blood sugar and electrolyte disturbances, which can exacerbate tremors and cognitive symptoms. Clear fluids and oral electrolyte solutions, along with small meals that combine carbohydrates and protein, help stabilize blood sugar and provide calories for healing.
Avoid stimulants and heavy, greasy foods to reduce gastrointestinal upset and improve medication tolerance. If a person cannot keep food or fluids down, seek clinical nutrition support to avoid further destabilization.
How a Supportive Environment Improves Comfort and Speeds Recovery
A calm, monitored environment with compassionate staff and minimal stimulation helps lower sympathetic overdrive and restore sleep, both of which support faster physical recovery during detox. Family members who follow clinical guidance can offer emotional support while clinicians maintain safety and medical oversight.
Close observation allows earlier medication adjustments and faster symptom resolution, making the transition to ongoing treatment smoother. For help with evaluation or admission to a supervised outpatient program in Massachusetts, contact Charles River Recovery admissions for an assessment and next steps.
Frequently Asked Questions
What Complications Can Arise from Alcohol Withdrawal?
Alcohol withdrawal can cause serious complications, including seizures, delirium tremens (DTs), and severe autonomic instability. Seizures most often occur within 24–72 hours and can cause injury or death without treatment.
DTs involve confusion, hallucinations, fever, and cardiovascular instability and can be life-threatening. Severe dehydration and electrolyte imbalance can also harm the heart and kidneys, so medical supervision during detox is critical.
How Can Family Members Support Someone Through Alcohol Detox?
Family support is vital. Offer calm emotional support, help arrange medical evaluation, and follow clinical instructions about visitation and care. Being patient, keeping communication open, and assisting with logistics, transportation, appointments, and aftercare planning can reduce stress and improve safety during detox.
What Role Does Nutrition Play in Alcohol Detox?
Nutrition helps stabilize blood sugar, replace lost nutrients, and support overall recovery. Small, frequent meals with protein and carbohydrates supply energy and promote healing. Hydration, including electrolyte solutions, is essential to prevent dehydration and correct imbalances. Good nutrition complements medical treatment and can reduce withdrawal severity.
Can Alternative Therapies Help During Alcohol Detox?
Alternative therapies, mindfulness, gentle yoga, and acupuncture, can complement medical care by reducing anxiety and improving well-being. Behavioral therapies like cognitive-behavioral therapy (CBT) address underlying patterns related to alcohol use. These approaches should not replace medical detox but can be integrated into a comprehensive plan after stabilization.
Disclaimer:
This article is for general information only and does not replace professional medical, legal, financial, or insurance advice. Policies, prices, and coverage vary. Always consult qualified professionals and your specific provider before making decisions.
Reference
- https://americanaddictioncenters.org/alcohol/withdrawal-detox
- https://en.wikipedia.org/wiki/Alcohol_withdrawal_syndrome
- https://medlineplus.gov/ency/article/000766.htm
- https://medlineplus.gov/ency/article/001552.htm
- https://www.aafp.org/pubs/afp/issues/2004/0315/p1443.html
- https://americanaddictioncenters.org/alcohol/withdrawal-detox
- https://www.asam.org/quality-care/clinical-guidelines/alcohol-withdrawal-management-guideline
- https://www.ccjm.org/content/83/1/67
- https://medlineplus.gov/ency/article/002149.htm

